Rheumatoid Arthritis Test Results: How Early Diagnosis Helps in Managing RA
What is Rheumatoid Arthritis?
Rheumatoid arthritis (RA) is a chronic autoimmune condition affecting the joints, causing inflammation, pain, and eventually joint damage. Early diagnosis is crucial for managing the progression of the disease, and the rheumatoid arthritis test plays a pivotal role in this. In this blog, we dive into the different types of blood tests used to diagnose rheumatoid arthritis, how they work, and what the results mean for early detection and treatment.
Common rheumatoid arthritis symptoms include:
- Joint pain and swelling
- Morning stiffness lasting more than 30 minutes
- Fatigue and loss of energy
- Fever and weight loss in advanced stages
If you’re experiencing any of these rheumatoid arthritis symptoms, it’s important to consider diagnostic testing as part of a broader health checkup. Check out our health checkup packages to find one that fits your needs.
What is the main cause of rheumatoid arthritis?
Rheumatoid arthritis is primarily caused by an overactive immune system that mistakenly attacks the body’s own joint tissues. This autoimmune response triggers inflammation and can eventually lead to joint damage if left untreated.
Several key factors contribute to developing rheumatoid arthritis:
Genetics plays a significant role – if someone in your family has RA, you may be more likely to develop it. However, having these genes doesn’t guarantee you’ll get RA; they just make you more susceptible.
Environmental triggers often act as the spark that sets off RA in people who are genetically susceptible. These triggers can include:
- Exposure to certain infections or viruses
- Long-term smoking
- Physical or emotional stress
- Obesity
- Environmental pollutants
Hormonal changes may explain why women are more likely to develop RA than men. Major hormonal shifts, such as those during pregnancy or menopause, can trigger the onset of RA or affect its severity.
Your lifestyle and habits can also influence both the development and severity of RA. Poor diet, lack of physical activity, and chronic stress may contribute to inflammation in your body, potentially triggering or worsening RA symptoms.
Understanding these causes helps healthcare providers develop more effective treatment strategies and helps patients make informed lifestyle choices to better manage their condition.
What Are the 4 Stages of Rheumatoid Arthritis?
RA progresses through four stages, each affecting the joints differently:
- Stage 1: Synovitis – Inflammation without visible joint damage.
- Stage 2: Moderate RA – Cartilage damage begins, causing pain and stiffness.
- Stage 3: Severe RA – Extensive cartilage and bone damage.
- Stage 4: End-stage RA – Complete joint destruction and deformities.
What is the best way to manage rheumatoid arthritis?
The most effective way to manage rheumatoid arthritis is through a comprehensive treatment approach that combines medication, lifestyle changes, and regular medical monitoring. Early diagnosis and treatment are crucial for preventing joint damage and maintaining quality of life.
Lifestyle Modifications
Simple daily adjustments can significantly impact your RA management:
- Regular gentle exercise, especially swimming or water aerobics, helps maintain joint flexibility
- Balanced diet rich in anti-inflammatory foods like fatty fish, nuts, and fresh fruits
- Adequate rest and stress management to prevent flare-ups
- Using assistive devices when needed to protect your joints
- Maintaining a healthy weight to reduce pressure on joints
Physical Therapy and Exercise
Working with a physical therapist can help you:
- Learn proper exercises to strengthen muscles around affected joints
- Improve flexibility and range of motion
- Develop better joint protection techniques
- Learn how to modify daily activities to reduce joint stress
Self-Care Strategies
Developing good self-care habits is crucial:
- Apply hot or cold therapy to affected joints
- Practice stress-reduction techniques like meditation or deep breathing
- Get adequate sleep to help manage fatigue
- Keep a symptom diary to track flare-ups and triggers
Medication Management
Working with your rheumatologist to find the right medication combination is essential. Modern RA treatments typically include:
- Disease-modifying antirheumatic drugs (DMARDs) to slow disease progression
- Anti-inflammatory medications to reduce pain and swelling
- Biologics for severe cases that don’t respond to traditional DMARDs
- Corticosteroids for temporary relief during flare-ups
Regular Medical Check-ups
Consistent monitoring of your condition helps:
- Track disease progression
- Adjust treatment plans as needed
- Catch complications early
- Monitor medication effectiveness and side effects
Medical History & Physical Examination in Rheumatoid Arthritis Diagnosis
Before ordering lab tests, doctors first assess medical history and conduct a physical examination to identify early signs of rheumatoid arthritis (RA). These steps help rule out other joint conditions and determine if further testing is necessary.
1. Medical History: Key Questions Your Doctor May Ask
A doctor will discuss your symptoms, lifestyle, and family history to assess RA risk. Some key questions include:
✔️ Symptom Onset & Progression:
- When did your joint pain and stiffness begin?
- Are the symptoms getting worse over time?
- Do you experience morning stiffness lasting more than 30 minutes?
✔️ Pain Pattern & Daily Impact:
- Is the pain affecting both sides of your body (symmetrical joint pain)?
- Does movement or mild exercise relieve stiffness?
- Do you feel fatigue, fever, or weight loss along with joint pain?
✔️ Family & Medical History:
- Does anyone in your family have RA or other autoimmune diseases?
- Do you have a history of smoking or long-term exposure to pollutants?
- Have you had any previous joint injuries or infections?
A detailed medical history helps doctors identify early RA symptoms and differentiate them from other joint disorders like osteoarthritis or lupus.
Types of Diagnosis for Rheumatoid Arthritis Test
Early diagnosis can prevent severe joint damage and improve long-term outcomes for those with RA. Various rheumatoid arthritis tests are available to detect markers of inflammation and autoantibodies that attack the body’s tissues.
1. Rheumatoid Factor (RF) Test
The rheumatoid arthritis test name most commonly associated with RA is the Rheumatoid Factor (RF) Test. This blood test checks for the presence of rheumatoid factor, an antibody found in about 80% of RA patients.
2. Anti-Cyclic Citrullinated Peptide (Anti-CCP) Test
The Anti-CCP test is more specific to RA than the RF test. People with a positive Anti-CCP test are more likely to have a severe form of RA, making it crucial for early rheumatoid arthritis diagnosis.
3. Erythrocyte Sedimentation Rate (ESR) and C-Reactive Protein (CRP) Tests
Both the ESR test and the CRP test measure the level of inflammation in the body. Higher levels indicate active inflammation, which is common in rheumatoid arthritis.
If you suspect any of these symptoms or need further clarification on diagnostic procedures, feel free to contact us for professional support and guidance.
How to Prepare for an Rheumatoid Arthritis Test?
Preparing for a Rheumatoid arthritis tests is generally straightforward, as most tests require minimal to no special preparation. Here’s what you need to know:
1. Blood Test:
Common rheumatoid arthritis tests include the Rheumatoid Factor (RF) test and the Anti-Cyclic Citrullinated Peptide (Anti-CCP) test. For these tests:
- No Special Preparations Needed: You can eat, drink, and continue your usual activities before the test.
- Medication Disclosure: Inform your healthcare provider about all medications, supplements, and herbs you’re taking, as some may influence test results.
2. Imaging Test:
If your doctor recommends imaging studies like X-rays, MRI, or ultrasound to assess joint condition:
- Follow Specific Instructions: Depending on the test, you might need to wear comfortable clothing or avoid metal accessories. Your healthcare provider will provide detailed instructions if any preparation is necessary.
3. General Tips:
- Medical History: Be prepared to discuss your symptoms, their onset, and any family history of arthritis. This information aids in accurate diagnosis.
- Stay Relaxed: Blood tests are routine procedures. If you’re anxious about needles, communicate this to the medical staff; they can offer support to make you comfortable.
By understanding the process and following any given instructions, you can ensure a smooth experience when undergoing tests for rheumatoid arthritis. Still have any questions, we have answered some common questions related to Rheumatoid Arthritis Test here – Rheumatoid Arthritis Blood Test
Complementary & Alternative Treatments for Rheumatoid Arthritis
While medical treatments like DMARDs and biologics remain the gold standard for managing rheumatoid arthritis (RA), many patients seek complementary and alternative therapies to ease symptoms, improve flexibility, and enhance overall well-being. These approaches should be used alongside, not as a replacement for, prescribed medications.
1. Acupuncture: Balancing the Body’s Energy
- Acupuncture, an ancient Chinese medicine practice, involves inserting thin needles into specific points on the body to stimulate nerves and improve blood circulation.
- Studies suggest that acupuncture may help reduce RA-related pain and inflammation by promoting the release of endorphins, the body’s natural painkillers.
- While acupuncture doesn’t cure RA, it can complement conventional pain management strategies.
2. Herbal Remedies: Nature’s Anti-Inflammatories
Certain herbs and natural supplements are believed to have anti-inflammatory properties that may benefit RA patients:
- Turmeric (Curcumin) – Contains curcumin, a natural anti-inflammatory that may reduce joint pain and swelling.
- Ginger – Has been shown to reduce inflammatory markers in arthritis patients.
- Boswellia (Indian Frankincense) – May help prevent the immune system from attacking joints.
- Green Tea – Contains polyphenols that can help slow cartilage destruction.
📌 Important Note: Always consult a doctor before taking herbal supplements, as they may interact with RA medications.
3. Mind-Body Practices: Yoga & Tai Chi for Joint Health
Practices like yoga and tai chi focus on gentle movement, flexibility, and stress reduction, which can significantly benefit RA patients.
✅ Yoga
- Improves joint mobility and reduces stiffness.
- Helps strengthen supporting muscles around joints.
- Reduces stress and inflammation levels through breathing techniques.
✅ Tai Chi
- A slow, low-impact martial art that enhances balance and flexibility.
- Shown to improve range of motion in RA patients.
- Encourages relaxation, reducing stress-related inflammation.
4. Massage Therapy & Hydrotherapy
- Massage therapy can improve circulation, reduce stiffness, and relieve muscle tension around affected joints.
- Hydrotherapy (warm water therapy) can ease joint pain by using heat and buoyancy to reduce pressure on inflamed joints.
5. Diet & Lifestyle Adjustments
A well-balanced anti-inflammatory diet can support RA management:
- 🍓 Eat: Omega-3-rich foods (salmon, flaxseeds), berries, nuts, and whole grains.
- 🚫 Avoid: Processed foods, excess sugar, and red meat (which may trigger inflammation).
A Holistic Approach to RA
Alternative therapies do not replace medical treatments but can be valuable add-ons for symptom relief and improved quality of life. Consult your rheumatologist before trying any new therapies to ensure they are safe and effective for you.
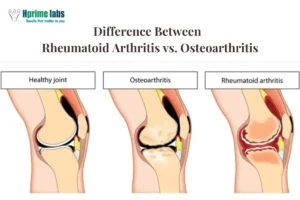
Rheumatoid Arthritis vs. Osteoarthritis: Key Differences in Diagnosis
Many people confuse rheumatoid arthritis with osteoarthritis due to overlapping symptoms. However, they are distinct:
- Rheumatoid arthritis is an autoimmune disease that affects the synovium (joint lining), causing inflammation and joint destruction.
- Osteoarthritis is a degenerative joint disease caused by wear and tear over time.
Blood tests, such as RF and Anti-CCP, help distinguish between rheumatoid arthritis vs osteoarthritis. For more comprehensive tests, you can visit one of our collection centers to undergo specialized diagnostic services.
What Is Worse: Rheumatoid Arthritis or Osteoarthritis?
When comparing what is worse, arthritis or osteoarthritis, rheumatoid arthritis (RA) is often considered more severe due to its autoimmune nature. RA can affect organs beyond the joints, making it more debilitating if left untreated. However, both conditions require early diagnosis to manage symptoms and prevent further damage.
Conclusion: Why Early Testing is Key to Managing Rheumatoid Arthritis
Timely diagnosis through rheumatoid arthritis tests like RF, Anti-CCP, ESR, and CRP can significantly impact treatment outcomes. If you are experiencing rheumatoid arthritis symptoms, contact a healthcare professional for early testing. Early intervention is crucial in managing the disease and maintaining a good quality of life.
We recommend checking our comprehensive health checkup packages to ensure you stay proactive about your health. For any assistance, you can also connect with us or visit one of our collection centers.






Leave a Comment